Long-Term Care Insurance Appeal
Purpose
This template provides a comprehensive framework for appealing the denial of a long-term care insurance (LTCI) claim, including the internal appeal process and external review options.
Important Notice
Act Quickly:
- Appeal deadlines are strict (often 60-180 days from denial)
- Check your denial letter for specific deadline
- Continue paying premiums to keep policy in force during appeal
Many Denials Are Overturned:
Initial claim denials are common, but many are successfully appealed with proper documentation and persistence.
Part 1: Policy and Claim Information
Policyholder Information
| Field | Information |
|---|---|
| Policyholder Name | _________________________________ |
| Date of Birth | _________________________________ |
| Social Security Number (last 4) | XXX-XX-_______ |
| Address | _________________________________ |
| City, State, ZIP | _________________________________ |
| Phone Number | _________________________________ |
| _________________________________ |
Policy Information
| Field | Information |
|---|---|
| Insurance Company | _________________________________ |
| Policy Number | _________________________________ |
| Policy Effective Date | _________________________________ |
| Group Policy (if applicable) | _________________________________ |
| Current Premium | $____________ / ____________ |
Claim Information
| Field | Information |
|---|---|
| Claim Number | _________________________________ |
| Date Claim Filed | _________________________________ |
| Date of Denial | _________________________________ |
| Type of Care Claimed | _________________________________ |
| Amount Claimed | $_________________________________ |
Care Provider Information
| Field | Information |
|---|---|
| Care Provider/Facility Name | _________________________________ |
| Address | _________________________________ |
| Phone | _________________________________ |
| Type of Care | ☐ Nursing Home ☐ Assisted Living ☐ Home Care ☐ Other |
| Care Start Date | _________________________________ |
Part 2: Denial Details
Denial Letter Review
☐ Denial letter received (Date: ___________)
☐ Denial letter attached to this appeal
Reason(s) for Denial (from denial letter)
☐ Does not meet benefit trigger requirements
☐ Does not meet Activities of Daily Living (ADL) criteria
☐ Cognitive impairment not substantiated
☐ Care is not from a qualified provider
☐ Elimination/waiting period not satisfied
☐ Pre-existing condition exclusion
☐ Policy lapsed for non-payment
☐ Care is not medically necessary
☐ Missing documentation
☐ Unauthorized provider/facility
☐ Service not covered under policy
☐ Other: _________________________________
Specific Language from Denial Letter
(Copy the exact reasons stated):
__________________________________________________________________
__________________________________________________________________
__________________________________________________________________
Policy Provisions Cited in Denial
| Provision | Page/Section | What It Says |
|---|---|---|
| _________________ | _________ | _________________________ |
| _________________ | _________ | _________________________ |
Part 3: Understanding Your Policy
Benefit Triggers
Most LTCI policies require meeting one of these benefit triggers:
ADL Trigger - Activities of Daily Living:
Policy requires inability to perform _____ ADLs (typically 2 of 6)
| ADL | Needs Assistance? | Documentation |
|---|---|---|
| Bathing | ☐ Yes ☐ No | ☐ Obtained |
| Dressing | ☐ Yes ☐ No | ☐ Obtained |
| Eating | ☐ Yes ☐ No | ☐ Obtained |
| Toileting | ☐ Yes ☐ No | ☐ Obtained |
| Transferring | ☐ Yes ☐ No | ☐ Obtained |
| Continence | ☐ Yes ☐ No | ☐ Obtained |
Cognitive Impairment Trigger:
☐ Substantial supervision required due to cognitive impairment
☐ Alzheimer's, dementia, or other cognitive condition diagnosed
Elimination Period (Waiting Period)
| Field | Information |
|---|---|
| Elimination period per policy | _______ days |
| Care start date | _________________ |
| Elimination period end date | _________________ |
| ☐ Elimination period satisfied |
Covered Services Per Policy
☐ Nursing home/skilled nursing facility
☐ Assisted living facility
☐ Adult day care
☐ Home health care
☐ Hospice care
☐ Respite care
☐ Other: _________________________________
Policy Maximums
| Benefit | Amount |
|---|---|
| Daily/monthly benefit | $____________ |
| Lifetime maximum | $____________ |
| Benefit period | ____________ years |
Part 4: Grounds for Appeal
Why the Denial is Wrong (check all that apply)
Eligibility Requirements Met:
☐ Claimant DOES meet ADL requirements (documentation attached)
☐ Claimant DOES have qualifying cognitive impairment (documentation attached)
☐ Elimination period HAS been satisfied (documentation attached)
☐ Pre-existing condition exclusion does NOT apply (documentation attached)
☐ Policy was in force at time of claim (documentation attached)
Care Provider/Service Issues:
☐ Provider IS qualified under policy terms
☐ Facility IS licensed as required
☐ Care IS medically necessary (physician statement attached)
☐ Service IS covered under policy terms
Documentation Issues:
☐ Required documentation IS now provided
☐ Insurance company failed to request additional documentation
☐ Documentation was already provided but not considered
Procedural Issues:
☐ Denial did not follow proper procedures
☐ Assessment was not conducted properly
☐ Relevant medical records not reviewed
☐ Company failed to obtain required information
Other:
☐ Other grounds: _________________________________
Part 5: Supporting Documentation Checklist
Medical Documentation
☐ Attending physician statement (completed by treating doctor)
☐ Medical records supporting need for care
☐ Cognitive assessment results (if cognitive impairment claimed)
☐ Functional assessment/ADL evaluation
☐ Plan of care from healthcare provider
☐ Hospital discharge summary (if applicable)
☐ Nursing notes documenting care needs
☐ Therapy notes (PT, OT, Speech)
ADL Documentation
☐ Detailed description of assistance needed for each ADL
☐ Care logs showing actual assistance provided
☐ Assessment from physician documenting ADL limitations
☐ Assessment from licensed healthcare professional
Provider Documentation
☐ Facility license
☐ Provider credentials/certifications
☐ Care provider agreement/contract
☐ Itemized bills for services provided
Policy Documentation
☐ Copy of insurance policy
☐ Certificate of coverage
☐ Any policy amendments or riders
☐ Premium payment records
Correspondence
☐ Original claim submission
☐ Denial letter
☐ All correspondence with insurance company
☐ Notes from phone calls (dates, names, what was said)
Part 6: Internal Appeal Process
Step 1: Review Denial and Deadline
☐ Reviewed denial letter thoroughly
☐ Identified specific reasons for denial
☐ Noted appeal deadline: _______________
☐ Identified what documentation is needed
Step 2: Gather Supporting Documents
☐ Obtained medical records
☐ Obtained physician statements
☐ Gathered care documentation
☐ Reviewed policy terms
Step 3: Write Appeal Letter
☐ Addressed each reason for denial
☐ Cited specific policy provisions
☐ Included supporting documentation
☐ Met formatting requirements
Step 4: Submit Appeal
☐ Appeal submitted before deadline
☐ Sent by certified mail, return receipt requested
☐ Kept copy of everything submitted
☐ Noted confirmation/tracking number
Appeal Submission Information
| Field | Information |
|---|---|
| Appeals Department Address | _________________________________ |
| Fax Number (if accepted) | _________________________________ |
| Phone Number | _________________________________ |
| Deadline to Appeal | _________________________________ |
| Date Appeal Submitted | _________________________________ |
| Method of Submission | _________________________________ |
| Tracking/Confirmation | _________________________________ |
Part 7: Internal Appeal Letter Template
[YOUR NAME]
[YOUR ADDRESS]
[CITY, STATE ZIP]
[PHONE]
[EMAIL]
[DATE]
[INSURANCE COMPANY NAME]
Appeals Department
[ADDRESS]
[CITY, STATE ZIP]
RE: APPEAL OF CLAIM DENIAL
Policyholder: [NAME]
Policy Number: [POLICY NUMBER]
Claim Number: [CLAIM NUMBER]
Date of Denial: [DATE]
Dear Appeals Committee:
I am writing to formally appeal the denial of my long-term care insurance claim dated [denial date]. I believe this denial was made in error, and I am providing additional documentation to support my claim.
POLICY INFORMATION:
- Policy Number: [Number]
- Effective Date: [Date]
- Type of Care: [Nursing home/assisted living/home care]
- Care Start Date: [Date]
- Daily Benefit: $[Amount]
DENIAL REASON:
According to your letter dated [date], my claim was denied because:
[Quote exact language from denial letter]
WHY THE DENIAL IS INCORRECT:
[Address each reason for denial specifically. Examples:]
1. Regarding Activities of Daily Living (ADL) Requirements:
Your denial states that I do not meet the ADL trigger requirement of needing assistance with [number] ADLs. However, as documented in the attached physician statement and medical records, I require substantial assistance with the following ADLs:
- Bathing: [Describe specific limitations and assistance needed]
- Dressing: [Describe specific limitations and assistance needed]
- [Other ADLs]: [Describe]
The attached functional assessment from Dr. [Name] dated [date] confirms that I meet the policy's benefit trigger requirements.
2. Regarding [Second Denial Reason]:
[Address with specific facts and documentation]
3. Regarding [Third Denial Reason, if applicable]:
[Address with specific facts and documentation]
POLICY PROVISIONS:
Under my policy, benefits are payable when [cite specific policy language]. As demonstrated by the enclosed documentation, I meet these requirements because [explain].
ENCLOSED DOCUMENTATION:
I am enclosing the following documents in support of this appeal:
1. [List each document]
2. [Continue listing]
3. [Continue listing]
REQUEST:
Based on the above, I respectfully request that you:
1. Reverse the denial of my claim
2. Approve benefits effective [date]
3. Process payment for services rendered
Please acknowledge receipt of this appeal and provide a written decision within the timeframe required by [state] law.
If you require any additional information, please contact me immediately at [phone] or [email].
Thank you for your prompt attention to this matter.
Sincerely,
_________________________________
[Your Signature]
[Your Printed Name]
Enclosures: [List all attachments]
cc: [Your attorney, if applicable]
[State Insurance Department, if applicable]
Part 8: If Internal Appeal is Denied
External Review Options
If your internal appeal is denied, you may have additional options:
State Insurance Department Review:
☐ File complaint with state insurance commissioner
☐ Request external review (if available in your state)
Independent External Review:
☐ Some states require insurers to offer external review
☐ Review is conducted by independent third party
☐ Decision is usually binding on insurer
Legal Action:
☐ Consult with attorney about lawsuit
☐ Consider small claims court for smaller amounts
☐ Explore bad faith insurance claims
State Insurance Department
| Field | Information |
|---|---|
| Department Name | _________________________________ |
| Phone | _________________________________ |
| Website | _________________________________ |
| Complaint Form | _________________________________ |
Filing a Complaint with State Insurance Department
What to Include:
☐ Copy of policy
☐ Copy of claim and denial
☐ Copy of appeal and response
☐ Description of issue
☐ Requested resolution
Part 9: Complaint Letter to State Insurance Department
[DATE]
[STATE] Department of Insurance
Consumer Complaints Division
[ADDRESS]
[CITY, STATE ZIP]
RE: Complaint Against [INSURANCE COMPANY]
Policyholder: [NAME]
Policy Number: [NUMBER]
Dear Insurance Commissioner:
I am filing a complaint against [Insurance Company] regarding their wrongful denial of my long-term care insurance claim.
POLICY INFORMATION:
- Insurance Company: [Name]
- Policy Number: [Number]
- Type of Policy: Long-Term Care Insurance
- Issue: Wrongful claim denial
SUMMARY OF COMPLAINT:
[Provide a clear summary of what happened, including:
- When you filed the claim
- The reason for denial
- Your appeal efforts
- Why you believe the denial is wrong]
CHRONOLOGY OF EVENTS:
[Date] - Began receiving long-term care at [facility/home]
[Date] - Filed claim with [Insurance Company]
[Date] - Received denial letter stating [reason]
[Date] - Filed internal appeal with supporting documentation
[Date] - Appeal denied because [reason]
[Present] - Filing this complaint
POLICY PROVISIONS:
My policy provides coverage for [describe coverage]. Under the terms of my policy, benefits are triggered when [describe trigger]. I meet these requirements because [explain].
REQUEST:
I request that the Department of Insurance:
1. Review my complaint
2. Investigate [Insurance Company]'s denial practices
3. Order [Insurance Company] to pay my claim
4. Take any other appropriate action
ENCLOSED DOCUMENTS:
1. Copy of insurance policy
2. Claim submission documents
3. Denial letter
4. Appeal letter and supporting documents
5. Appeal denial letter
6. [Other relevant documents]
Thank you for your assistance.
Sincerely,
_________________________________
[Your Signature]
[Your Name]
[Address]
[Phone]
[Email]
Part 10: Common Denial Reasons and Responses
"Does Not Meet ADL Requirements"
Response Strategy:
☐ Obtain detailed physician statement documenting each ADL limitation
☐ Get functional assessment from licensed healthcare professional
☐ Provide care logs showing actual assistance provided
☐ Include specific examples of what happens without assistance
"Cognitive Impairment Not Substantiated"
Response Strategy:
☐ Obtain neurological or psychiatric evaluation
☐ Provide cognitive testing results (MMSE, MoCA, etc.)
☐ Include diagnosis of dementia, Alzheimer's, or related condition
☐ Document need for substantial supervision
"Provider Not Qualified"
Response Strategy:
☐ Verify provider meets policy requirements
☐ Obtain provider's license and credentials
☐ Show provider is same type as specified in policy
☐ Request policy definition of "qualified provider"
"Elimination Period Not Satisfied"
Response Strategy:
☐ Document exact care start date
☐ Provide calendar showing days of care
☐ Clarify what counts toward elimination period in your policy
☐ Include invoices/records showing continuous care
"Pre-Existing Condition"
Response Strategy:
☐ Determine policy's pre-existing condition period
☐ Show condition was disclosed on application
☐ Demonstrate current need is unrelated to pre-existing condition
☐ Show pre-existing condition exclusion period has passed
"Care Not Medically Necessary"
Response Strategy:
☐ Obtain physician statement of medical necessity
☐ Include detailed care plan
☐ Document what would happen without care
☐ Show care is prescribed by physician
Part 11: Appeal Timeline Tracking
Key Dates
| Event | Date | Notes |
|---|---|---|
| Care began | ____________ | |
| Claim filed | ____________ | |
| Denial received | ____________ | |
| Appeal deadline | ____________ | |
| Appeal submitted | ____________ | |
| Expected response | ____________ | |
| Response received | ____________ |
Communication Log
| Date | Contact | Method | Summary |
|---|---|---|---|
| _______ | _____________ | ☐ Phone ☐ Mail ☐ Email | _________________ |
| _______ | _____________ | ☐ Phone ☐ Mail ☐ Email | _________________ |
| _______ | _____________ | ☐ Phone ☐ Mail ☐ Email | _________________ |
| _______ | _____________ | ☐ Phone ☐ Mail ☐ Email | _________________ |
Part 12: Getting Help
Professional Assistance
Long-Term Care Insurance Specialists:
- American Association for Long-Term Care Insurance (AALTCI)
- Website: aaltci.org
- Claims assistance programs available
Elder Law Attorneys:
☐ Can review denial and policy
☐ Can handle appeals and litigation
☐ May work on contingency for wrongful denials
Insurance Bad Faith Attorneys:
☐ Specialize in insurance company misconduct
☐ May recover additional damages
State Resources:
☐ State Insurance Department consumer assistance
☐ State SHIP (State Health Insurance Assistance Program)
☐ Legal aid organizations
Questions to Ask an Attorney
☐ Do you handle long-term care insurance disputes?
☐ What is your experience with appeals?
☐ What are my chances of success?
☐ What are your fees?
☐ Do you work on contingency?
☐ What additional damages might be available?
Part 13: Protecting Your Rights
During the Appeal Process
☐ Continue paying premiums - Don't let policy lapse
☐ Keep all documents - Create copies of everything
☐ Document all communications - Note dates, names, content
☐ Meet all deadlines - Appeals have strict time limits
☐ Send by certified mail - Get proof of delivery
☐ Request everything in writing - Don't rely on verbal promises
Know Your Rights
☐ Right to appeal denial
☐ Right to receive denial in writing with reasons
☐ Right to review your claim file
☐ Right to external review (in many states)
☐ Right to file complaint with state insurance department
☐ Right to sue for benefits and potentially bad faith
Part 14: Resources
Insurance Company Contact
| Field | Information |
|---|---|
| Company Name | _________________________________ |
| Claims Phone | _________________________________ |
| Appeals Address | _________________________________ |
| Appeals Fax | _________________________________ |
State Insurance Department
| Field | Information |
|---|---|
| Name | _________________________________ |
| Consumer Hotline | _________________________________ |
| Website | _________________________________ |
Professional Resources
| Resource | Contact |
|---|---|
| AALTCI Claims Help | aaltci.org |
| State SHIP Program | _________________________________ |
| Elder Law Attorney | _________________________________ |
| Legal Aid | _________________________________ |
Signatures
Appellant Certification:
I certify that the information in this appeal is true and accurate to the best of my knowledge.
Signature: _________________________________ Date: _______________
Print Name: _________________________________
This template is for informational purposes only and does not constitute legal advice. Consult with an attorney or insurance professional for specific guidance on your long-term care insurance claim.
Do more with Ezel
This free template is just the beginning. See how Ezel helps legal teams draft, research, and collaborate faster.
AI that drafts while you watch
Tell the AI what you need and watch your document transform in real-time. No more copy-pasting between tools or manually formatting changes.
- Natural language commands: "Add a force majeure clause"
- Context-aware suggestions based on document type
- Real-time streaming shows edits as they happen
- Milestone tracking and version comparison
Research and draft in one conversation
Ask questions, attach documents, and get answers grounded in case law. Link chats to matters so the AI remembers your context.
- Pull statutes, case law, and secondary sources
- Attach and analyze contracts mid-conversation
- Link chats to matters for automatic context
- Your data never trains AI models
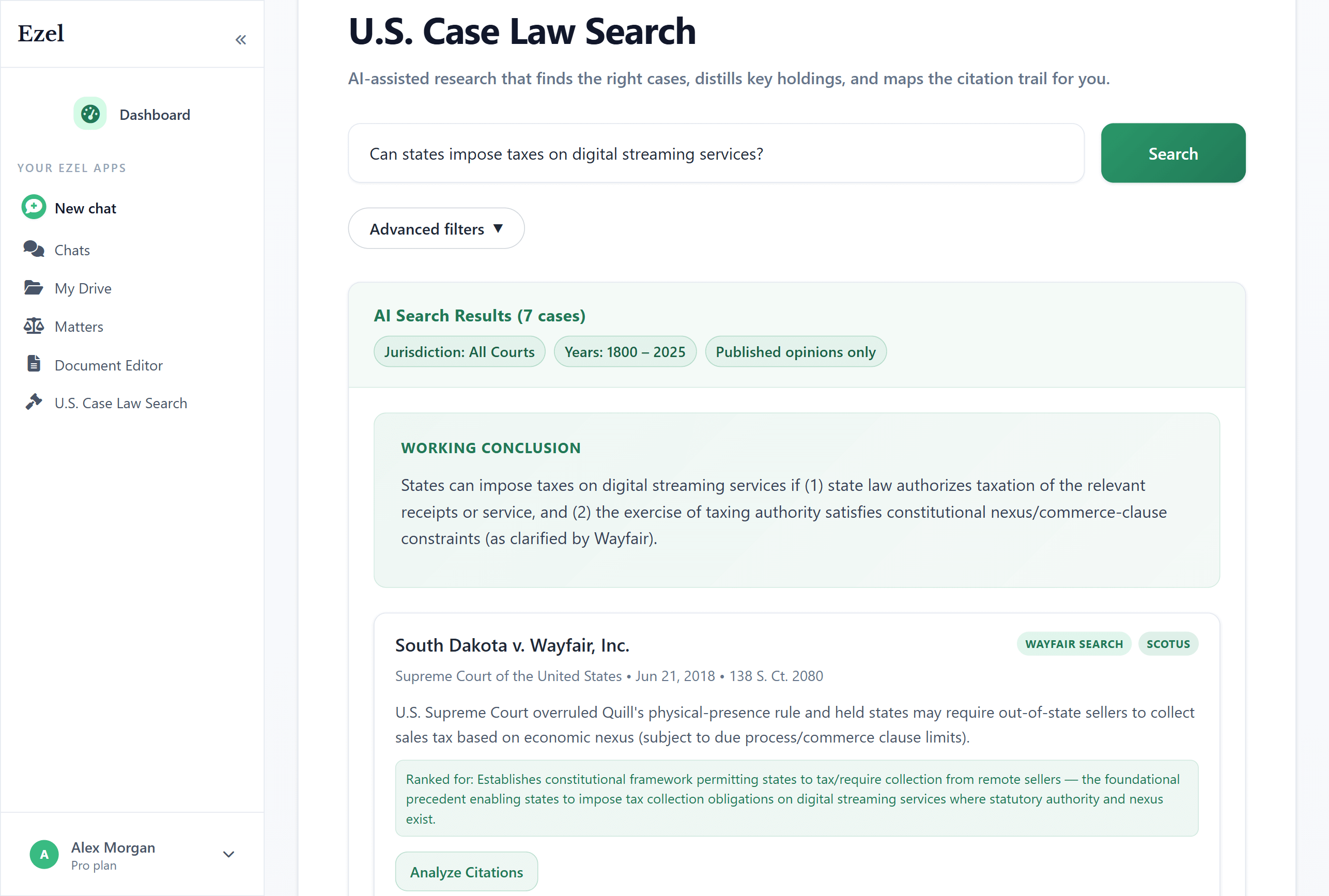
Search like you think
Describe your legal question in plain English. Filter by jurisdiction, date, and court level. Read full opinions without leaving Ezel.
- All 50 states plus federal courts
- Natural language queries - no boolean syntax
- Citation analysis and network exploration
- Copy quotes with automatic citation generation
Ready to transform your legal workflow?
Join legal teams using Ezel to draft documents, research case law, and organize matters — all in one workspace.